
Herpes Zoster (Shingles) and Eyes
December 10, 2021

Most people either had chickenpox as a child or got the vaccine at some point. The chickenpox virus is called varicella zoster virus, which is a member of the herpes virus family (Not all herpes viruses are sexually transmitted diseases). It is estimated that 90-95% of adults in the United States have varicella zoster virus antibodies from prior exposure.
Herpes Zoster Virus
While the acute case of chickenpox eventually resolves, the virus never fully leaves the body, but rather stays dormant until an opportune time to reappear occurs. When the virus reactivates later in life, it presents as “shingles.” A shingles outbreak can occur on the torso, head, and face. It typically respects the midline and only affects one side of the body. When shingles affects the eyes, it is called herpes zoster ophthalmicus. This is due to a reactivation of the varicella zoster virus in the ophthalmic division of the trigeminal nerve, which is responsible for innervating the forehead, cornea, upper check, and tip of the nose.
Risk Factors for Herpes Zoster
The status of the immune system is one of the biggest risk factors for developing shingles. The body is typically able to control the latent virus until a triggering event happens that weakens the body’s immune system. When the function of the immune system is decreased due to extreme stress, immunosuppressive medications, or immunocompromised conditions, such as HIV, the zoster virus takes advantage of the opportunity to present itself again. The risk of shingles also increases in people over the age of 60 years old.
Signs & Symptoms of Herpes Zoster
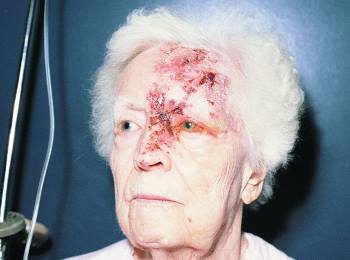
Shingles has a prodrome phase, which is equivalent to a warning sign that the body is trying to fight something. This typically involves a combination of the following: fever, fatigue, headache, eye pain, and pain along the affected nerve path.
Once in the active phase, red and painful vesicles appear along the affected nerve or “dermatome.” It might have a rash-like, blistered appearance with associated swelling. The vesicles ooze a clear discharge, which eventually scabs and may cause scarring. Hutchinson’s sign is the presence of a lesion on the tip of the nose that has a strong correlation to corneal involvement, due to the shared pathway of nerves.
Ocular symptoms include foreign body sensation (feels like there is something in the eye), eye pain, watering, blurry vision, and photophobia (light sensitivity). If there is corneal involvement, the eye is typically red and the eyelid is swollen.
Diagnosis of Herpes Zoster
A slit lamp examination is necessary to look for corneal involvement. This can range from small areas of dryness or irritation to severe corneal swelling. The sensitivity of the cornea is usually decreased during an acute episode of ocular herpes zoster. Corneal sensitivity can be tested using a wisp of cotton from a cotton swab. Eyelid lesions are large enough to be viewed with adequate lighting and the naked eye. Herpes zoster rarely affects the retina or optic nerve.
Treatment of Herpes Zoster
Oral antiviral medications are the most important aspect of treatment for shingles. To decrease the risk of chronic complications, the medicine should be started as soon as possible. Even if the oral antivirals are prescribed by the primary care physician, the eyes should still be examined if there are lesions around the face or eyes. Artificial tears help sooth irritated eyes related to the virus. Other cases require topical steroid drops for corneal swelling or zoster-related uveitis. When the eye is severely involved, there is also a risk for glaucoma damage, so pressure-lowering drops are also prescribed in some cases.
In order to prevent a “bacterial superinfection,” the eyelid and facial lesions should be covered with antibiotic ointment. While the body’s immune system is compromised with herpes zoster, other germs can take advantage of the situation and cause a bacterial infection that wouldn’t happen otherwise.
The primary care physician will prescribe medication for nerve pain on an as needed basis, and hopefully minimizing chronic pain issues with postherpetic neuralgia. This is a long-term neuropathy that causes pain or tingling even after the viral infection has subsided. For those who suffer from postherpetic neuralgia, depression is a major concern that needs to be addressed for the overall well-being of the individual.
Preventing Herpes Zoster
Some people are prone to reactivation of the zoster virus during times of extreme stress or changes to the immune system. Maintenance therapy with antiviral medications is helpful to keep the virus under control for these individuals. A very effective varicella-zoster vaccination is available for those over 50 years old to prevent shingles and associated complications.