
Creepy Crawlies: Eye Infestations
November 6, 2020

Mites, lice, and parasites can inhabit the eyelashes and eyeball. These creepy crawlies are microscopic, but can wreak havoc on the health of the eyes. The following five conditions are the most common types of ocular infestations.
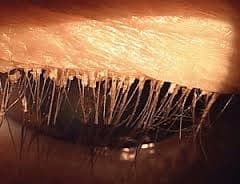
Demodex
Demodex are a type of parasitic mite that is located on human skin and typically does not cause problems unless overproduction of the organism occurs. The two main species are Demodex folliculorum and Demodex brevis. Shaped like a tiny worm with legs, these microscopic critters can infest the eyelashes more commonly in people over 60 years old. The mites burrow under the hair follicles and oil glands along the eyelid margin. In the process, they eat and damage skin cells around the hair follicle. This causes dandruff-like skin debris that looks like cylinders of oily skin flakes wrapped around each individual lash. The damage to the follicle can lead to misdirected growth and loss of lashes.
Symptoms of a Demodex infestation are similar to that of dry eye syndrome: itching, burning, foreign body sensation, and fluctuating vision. Usually, symptoms are worse upon waking in the morning after the mites are more active in the dark at night. The collection of oily skin debris clog the meibomian glands of the eyelids, which can cause hordeola, or styes, and blepharitis. Although the symptoms are similar to dry eyes, the treatment strategy for dry eyes will only provide a small amount of temporary relief for a true Demodex infestation. Until the mites are consistently treated, the reproductive cycle continues. There are prescription and non-prescription treatments that involve lid wipes and scrubs, most including tea tree oil. If the infestation is severe, some people may need to have the mites mechanically removed from the lashes in the office.
Lice
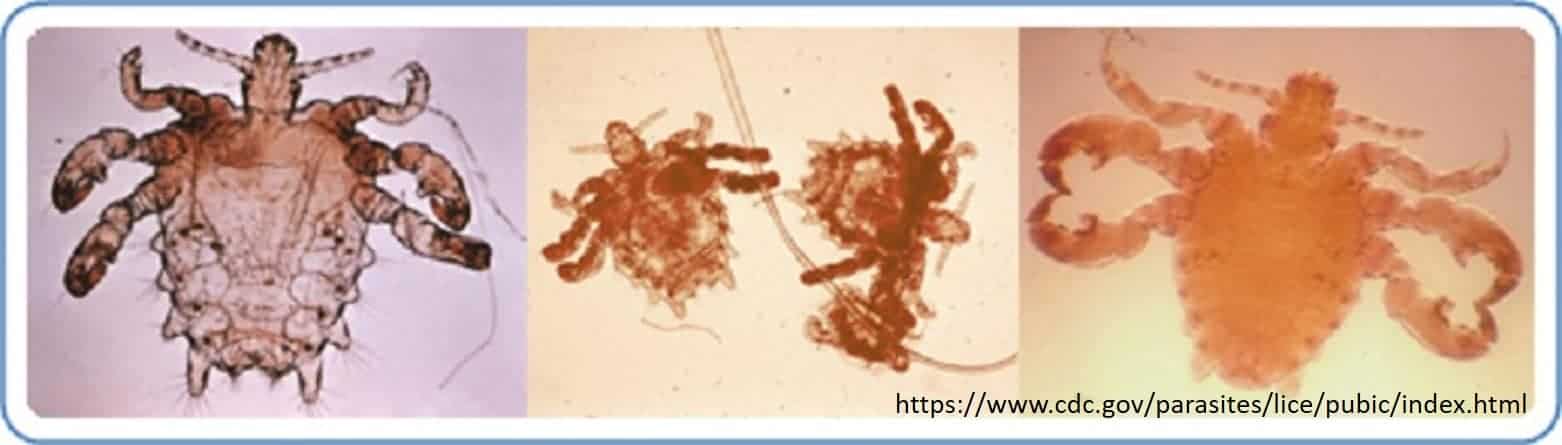
There are three different kinds of lice: head, body, and pubic. One of the main differences between the types of lice is the length of the body and legs based on the density of hair they inhabit. Surprisingly, the density or spacing of eyelash follicles is most similar to that of pubic hair, making it the second most suitable location for pubic lice to live. Therefore, pubic lice (Phthiriasis pubis) are the most common form of lice found in the eyelashes. It can be transferred by hand contact from the genitals to the eye or from contaminated bedding and towels.
Symptoms of a lice infection are itching, watering, and a crusty or sticky discharge in the eyelashes. The eyes may be red, and there could be black spots on the eyelid at the base of the eyelashes. These spots are actually particles of lice feces. A louse has three life stages: nit, nymph, and adult. In order to eliminate the bugs, they need to be removed at an eye doctor’s office for several consecutive days. Bland ophthalmic ointments can also be used on the eyelashes to “smother” the lice. Avoid using medicated shampoo on your eyelashes, as this may cause greater ocular irritation.
Acanthamoeba
Acanthamoeba is a single-celled free-living amoeba that is parasitic in nature. It is one of the most common organisms in the environment, but usually does not pose an ocular threat until it is placed on the eye. Fresh water bodies (lakes, ponds, creeks), soil, swimming pools, and hot tubs are the perfect habitats for Acanthamoeba. Most infections are seen in contact lens wearers after the person has worn the contacts in contaminated water or cleaned the lenses with a contaminated liquid.
Symptoms of an Acanthamoeba infection are pain, light sensitivity, foreign body sensation, cloudy vision, and tearing. Treatment involves intense topical therapies differing case by case. In order to protect against an infection, proper contact lens hygiene is crucial. Be sure to wash hands before inserting and removing contact lenses. Use fresh solution each day. Never sleep in contacts after swimming, and dispose contacts as directed by your eye doctor.
Toxoplasmosis
Toxoplasma gondii is a parasite that can infect both healthy and immunocompromised people. It causes the retinal condition, toxoplasmosis. Most healthy people do not have symptoms during an active infection because the immune system keeps the parasite to a minimum. If a woman becomes infected while pregnant, the infection can be transmitted to the fetus. The baby could be born with inflammation in the retina, which leads to permanent scarring and possible decreased vision. There are more serious life-threatening complications that can affect the nervous system of the baby, however, this is less common.
If an individual has congenital toxoplasmosis (i.e. they were born with it), it may not be diagnosed for several years if the child doesn’t have a dilated eye exam. The retinal scarring is permanent and can worsen if the parasite reactivates later in life. Since most cases are diagnosed years after the damage has occurred, there is no treatment other than addressing any associated retinal complications that may occur. The parasite can also be transmitted by eating raw or undercooked contaminated meat and accidental ingestion of cat litter or feces. Toxoplasma gondii can lay eggs in the intestinal tract of cats, which then contaminated the litter box. To minimize the risk of exposure, it is always best to let someone else change the litter box while pregnant.
Toxocariasis

The initial symptoms are blurred vision, pain, light sensitivity, and floaters that usually only affects one eye. The infection causes inflammation, or swelling, in the back of the eye, which can damage the retina. A retinal granuloma (or mass) is a common sign of toxocariasis that is visible once the pupils are dilated. If the inflammation and granuloma are severe, it may lead to a retinal detachment, causing permanent vision loss. Depending on the severity of the infection, surgery may be needed to removed the vitreous (gel-like substance inside the eye). The primary concern during an active infection is to treat the ocular inflammation, which is usually accomplished with eye injections. Systemic medication to treat the entire body is also an option in certain cases.
Resources:
https://www.reviewofoptometry.com/article/spotlight-on-demodex-eliminating-the-mitey-menace
https://www.cdc.gov/parasites/toxoplasmosis/
https://eyewiki.aao.org/Toxocariasis